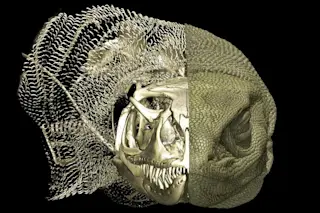
When one suffers a heart attack and doesn’t receive treatment fast enough, lack of oxygen can cause damage to cardiomyocytes — heart muscle cells — and they can begin to die off. Because humans can not grow new cardiomyocytes, this can cause scar tissue to form on the heart, preventing it from pumping as efficiently as it should. However, a recent study from a Max Delbrück Center for Molecular Medicine research team has found that zebrafish can regenerate cells and organs — even the heart.
“We wanted to find out how this little fish does that, and if we could learn from it,” says Jan Philipp Junker, in a press release. Junker along with Daniela Panáková — the study team leaders — simulated myocardial infarction injuries to zebrafish hearts. According to the study, now published in Nature Genetics, researchers tracked the regeneration of cardiomyocytes using single-cell analyses and cell lineage ...