Many people may be living life without a particular brain region – and not suffering any ill-effects.
In a new paper in Neuron, neuroscientists Tali Weiss and colleagues discuss five women who appear to completely lack olfactory bulbs (OB).
According to most neuroscience textbooks, no OB should mean no sense of smell, because the OB is believed to be a key relay point for olfactory signals. As Wikipedia puts it:
The olfactory bulb transmits smell information from the nose to the brain, and is thus necessary for a proper sense of smell.
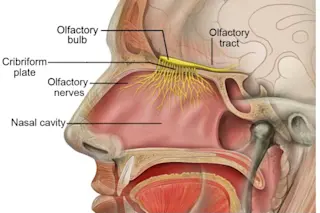
Scent molecules activate olfactory receptors and signals travel up the olfactory nerves to the olfactory bulb, and then on to the rest of the brain via the olfactory tract. From Wikipedia.
However, remarkably, Weiss et al.’s five women seem to have entirely normal sense of smell despite lacking any visible OBs on brain MRI scans. On both subjective ...