"Grandpa fell on knee. Two days before. Pain," the young woman said. Her wizened grandfather dozed on a stretcher.
"How are you, sir?" I inquired softly.
In loud Cantonese, the granddaughter repeated the question. She smiled apologetically. "No hear good."
His eyes fluttered open. When I palmed his right knee, he winced. The joint was swollen, the kneecap scuffed, but he didn't complain when I bent his knee. With the help of an interpreter, I learned that he tripped on his way to the bathroom two days ago.
"No dizziness? No passing out? Didn't hit his head?" I asked. A yes to any of these questions would suggest more serious heart or neurological problems.
"No," the granddaughter replied. "Only tripped."
"He feels OK now?"
"OK," she echoed.
The rest of his physical exam, except for weakness on his right side due to a previous stroke, was pretty darn good for an 85-year-old man.
His nurse appeared with the IV kit and blood tubes. "Admission labs?" she asked briskly.
"What makes you think he needs to come in?" I asked confidently.
"Grandpa fell," the nurse pointed out.
"It's his knee. Let's give him a Percocet. If the X-ray's negative, then he'll be good to go. We need the bed. And no Motrin, OK? He's already on Plavix and Persantine."
The latter two are potent anticlotting agents, and anti-inflammatory drugs like Motrin have a nasty way of making older stomachs bleed.
In the wild, animals past their prime face predictable perils: Old hippos starve when their teeth wear out; arthritic giraffes are felled by lions. For our bipedal species, the most dangerous environmental menace is gravity. Every year in the United States, one-third of people over 65 fall, risking not only a hip fracture but also a blow that can cause potentially deadly bleeding inside the skull. Compounding the risk for the elderly is the growing use of anticoagulants, which limit clot formation. Although these drugs help reduce the risk of strokes and heart attacks, they can turn a minor head contusion into a life-threatening gusher.
The patient's X-rays came back negative, as predicted. Hurrying into his cubicle, I announced, "Everything's OK—he can go home."
But the patient's visiting nurse had arrived to take over for the daughter. "So when will he go upstairs?" she asked.
"No, he doesn't need admission," I said.
Her brow furrowed. "You know, he has been falling a lot," she said carefully. "The family is worried."
My perkiness evaporated. A patient who frequently falls must be hospitalized to prevent further risk and to identify the reason for the unsteadiness. Frustratingly, the answer is usually nothing more than old age.
The nurse reappeared equipped with her IV paraphernalia.
"Let's get labs," I said. "And the usual head CT."
As the years go by, the adult brain slowly atrophies, like a desiccated orange detaching from its rind. The shrinkage can cause problems. Cerebral veins are tethered to the superior sagittal sinus, the large blood vessel that runs front to back along the underside of the skull. As the brain contracts, these bridging veins must stretch, making them vulnerable to shearing forces caused by rapid head movements or even modest contusions. Without sufficient brain tissue to support and compress the bleeding site, small, low-pressure venous leaks may go unstanched. The blood seeps into the gap between the arachnoid membrane that encloses the brain and the lining of the skull, or dura mater. Bleeding into this space is called a subdural hematoma.
Acute subdural hematomas result from severe head trauma and expand quickly. Chronic subdural hematomas, on the other hand, often spread slowly—and without visible symptoms. What really scares emergency physicians—and has me repeating to patients and their families, "Return if there's any change in behavior"—is that older people who have fallen can look fine for weeks before the bleeding causes symptoms. By then, relatives will have forgotten the long-ago head knock, attributing Granddad's confusion to the heat, the cold, or a dizzy spell. Without that critical, sometimes lifesaving clue, precious time is lost.
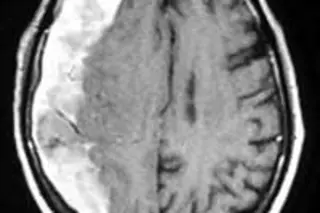
Forty-five minutes later, the radiologist called. "Your patient has a big subdural on the right. Evidence of old bleeding too. How is he doing?"
I was shocked. "He looked great to me. I thought the CT was a waste."
I hurried to the patient's room. The nurse was already there. "Big subdural," I said.
"Oh, gosh," she exclaimed. "Let's get him into a monitored bed."
As soon as we sat him up, the patient vomited. Nausea is a worrisome sign that increasing pressure is irritating the brain. Now I was in a hurry. If the enlarging hematoma pressed on his brain too much, the patient would suffer permanent damage.
The neurosurgeon hadn't called back. How much time had I wasted over that silly knee? I rushed upstairs and headed over to the surgery office.
"I need a neurosurgeon," I said, panting.
The secretary got on the phone. "I'll do what I can, Dr. Dajer."
No one answered her pages.
"Please keep trying," I pleaded.
Back downstairs, I found the patient tracing circles with his finger, signaling "dizzy."
"Blood pressure's going up," the nurse announced.
I started to sweat. From a hydraulics perspective, the brain is a bowl of jelly honeycombed with high-pressure pipes. Whenever blood pressure in the brain rises too much, the brain senses that it's running short on blood flow and provokes an even higher blood pressure, which in turn prompts more bleeding. "Two hours, two whole hours wasted," I kept repeating in silent self-flagellation.
Aside from surgery, there are two techniques to reduce intracranial pressure temporarily. One involves intubating the patient and giving artificial respiration. That reduces the level of carbon dioxide in the blood, which causes arteries to contract, thus shrinking overall brain volume. The second method is to give mannitol, a complex sugar, intravenously, which shrinks brain tissue by drawing water out of brain cells. Each technique buys time, and each has side effects.
"Surgery, five-oh-two-five," our clerk called out.
I grabbed the handset.
"Surgery." It was the resident, not the chief surgeon.
"Listen, I've got a subdural down here," I said. "Not doing well. The on-call surgeon hasn't answered. Can you guys at least notify the OR and get things rolling?"
"Let me take a look, OK?
"Ten long minutes later, the surgeon phoned. "How are you?" he drawled, as laid-back as an airline pilot reading the altitude. "I was in the OR. Whatcha got?"
I spilled my story.
"We'll get him up," the surgeon said.
The patient stayed conscious and kept answering our questions. The old guy's brain was durable.
In the operating room, the neurosurgeon drilled four small holes in the skull, sawed between them, and lifted off a rectangle of bone the size of a credit card. The dura mater beneath was tense and black, bulging with clotted blood. The surgeon incised twice to make an X, allowed the accumulated blood to pour out, then carefully irrigated the surface of the brain while looking for signs of persistent bleeding. When everything looked good, he placed a flat rubber drain inside the incision, replaced the bone flap, stitched the scalp closed, and stapled the skin shut. Done.
Three days later, the patient was out of intensive care. Four days after that, he was in his new digs: a nursing home.
"So he did well?" the nurse asked when I gave her the follow-up.
"Amazingly," I replied. "That subdural was so big it would have killed you or me." I shook my head. "Chief complaint: two-day-old knee pain. And he looked so good. . . ."
"Don't beat yourself up." She grinned. "Around here, it's always the ones you don't worry about that you have to worry about. But that's just a nurse's opinion."
Tony Dajer is interim chief of the emergency department at New York University Downtown Hospital. The cases described in Vital Signs are true stories, but the authors have changed some details about the patients to protect their privacy.