On average, the residents of Sun City, Arizona, occupy their domiciles for a dozen years. When they depart—almost always by dying—they often leave their brains behind. The stages of physical and mental decline take them from their dream house to a hospital off Del Webb Boulevard, then to a nursing home, and finally back to the medical complex, where researchers harvest their most important organ. Hoping to do good for science, they have enrolled in the Brain and Body Donation Program of the Banner Sun Health Research Institute—widely considered the world’s preeminent brain bank.
The Crack Team That Removes & Preserves People's Brains Just Hours After They Die
An Arizona retirement community helps create the world’s greatest brain bank.
Oct 16, 2012 5:00 AMNov 12, 2019 5:26 AM
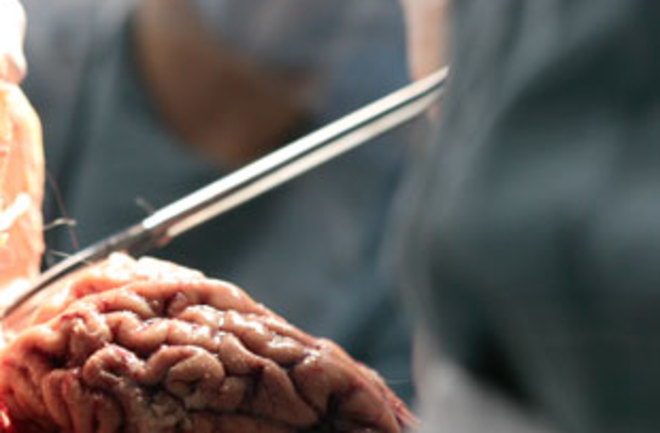
Doctors recover tissue during an autopsy at the institute in Sun City. | Courtesy Banner Sun Health Research Institute
Newsletter
Sign up for our email newsletter for the latest science news
0 free articles left
Want More? Get unlimited access for as low as $1.99/month
Stay Curious
Sign up for our weekly newsletter and unlock one more article for free.
View our Privacy Policy
Want more?
Keep reading for as low as $1.99!
Already a subscriber?
Find my Subscription
More From Discover
Stay Curious
Subscribe
To The Magazine
Save up to 40% off the cover price when you subscribe to Discover magazine.
Copyright © 2025 LabX Media Group
