RYGER/Shutterstock
Bionic eyes seem the stuff of science fiction. But not only are they real, they keep improving: A new technique has the potential to help patients with retinal implants see better, indoors and out.
People who have lost their vision due to a degenerative eye condition can have it partially restored with this technology. Retinal implants, chips of electrodes inserted in the retina, work by electrically stimulating a patient’s remaining retinal cells directly, rather than letting light waves do it.
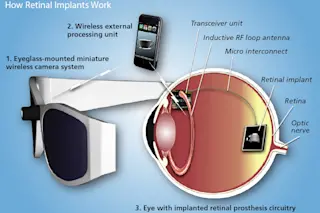
An external camera mounted within glasses captures an image and feeds it to a simple microprocessor — typically worn somewhere on the body, like a belt — which then wirelessly transmits a set of instructions to the electrodes in an implant. Those electrodes then re-create the image in grainy black and white within the eye’s retinal cells. Presto, electronic eyesight. Relying on them indoors, where one can make out ...