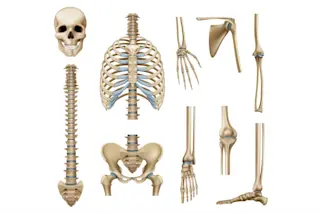
A 17th-century Russian nobleman named Butterlijn had a bone to pick with his surgeon. Butterlijn, the story goes, had been struck in the head with a sword, and his surgeon repaired the injury by transplanting a piece of dog bone into Butterlijn’s skull. He survived, only to be excommunicated by his church because he was deemed no longer fully human. Butterlijn demanded that the surgeon take the dog bone back out; when the surgeon tried, he found that Butterlijn’s skull had regrown around it. By some accounts, it was the first successful bone transplant.
People have been using foreign materials to repair damaged bones for millennia — there’s evidence of patch jobs in Neolithic Peru and ancient Egypt, though they used other materials like gold and iron instead of actual bone. While Butterlijn is the first person we know of to receive an actual donated bone, he was far from ...