At first, no one noticed that Joe Borelli was losing his mind — no one, that is, but Borelli himself. The trim, dark-haired radiologist was 43 years old. He ran two practices, was an assistant professor at the Medical University of South Carolina and played a ferocious game of tennis. Yet he began to have trouble recalling friends’ names, forgot to run important errands and got lost driving in his own neighborhood. He’d doze off over paperwork and awaken with drool dampening his lab coat.
Borelli feared he had a neurodegenerative disease, perhaps early onset Alzheimer’s. But as a physician, he knew that memory loss coupled with fatigue could also indicate obstructive sleep apnea (OSA), a disorder in which sagging tissue periodically blocks the upper airway during slumber. The sufferer stops breathing for seconds or minutes, until the brain’s alarm centers rouse him enough to tighten throat muscles. Although the cycle may repeat hundreds of times a night, the patient is usually unaware of any disturbance.
Borelli checked in to a sleep clinic for tests, which came out negative. He went to a neurologist, who found nothing wrong. At another sleep clinic, Borelli was diagnosed with borderline OSA; the doctor prescribed a CPAP (continuous positive airway pressure) machine, designed to keep his airway open by gently inflating it. But he still awoke feeling exhausted, and he quit using the device after a couple of months.
Borelli’s fingers soon grew so clumsy that he couldn’t button his shirt cuffs. He was easily winded, and his heart raced whenever he rose from a chair. He developed chronic severe anxiety. He gave up tennis and his chairmanship of a national professional committee. His marriage fell apart. He contemplated suicide. “One day,” he recalls, “I collapsed in the shower, crying.” Then he went looking for the best sleep specialist in America.

Joe Borelli, at home with a CPAP machine that helps him breathe, experienced years of fatigue and cognitive impairment due to an undiagnosed sleep disorder. Now healthy, he has created the SleepMapper app to help other CPAP users monitor the quality of their sleep. Sean Rayford
He settled on Christian Guilleminault, a venerated clinician and researcher at Stanford Medical School, who diagnosed him with upper-airway resistance syndrome (UARS), a condition in which the airway is partially obstructed during sleep. Unlike full-blown apnea, UARS — which is much harder to detect — restricts breathing rather than stopping it. But both conditions, which prevent a person from sleeping deeply for any length of time, can trigger ailments ranging from cognitive deficits to hypertension.
“You’ve had this your entire life,” Guilleminault declared before putting Borelli back on a CPAP at more than twice the air pressure as before.
Borelli hoped desperately that Guilleminault could cure him. Getting a good night’s sleep had become a matter of life and death.
A National Sleep Crisis
The first sleep-research lab opened in 1925 at the University of Chicago. Yet until fairly recently, scientists focused more on describing the phenomenon — its stages, aberrations and basic physiology — than on understanding its purpose. No one could really say what sleep was for, or even whether it was absolutely necessary.
Over the past couple of decades, however, researchers have been closing in on the whys of sleep, largely by studying what happens when organisms are deprived of it. A growing stack of evidence suggests that sleep is central to the health of both body and mind, regulating processes ranging from memory to metabolism.
These findings take on added urgency because we’re experiencing a national sleep crisis. According to the National Institutes of Health, up to 70 million Americans have a serious sleep disorder — including chronic insomnia as well as sleep apnea and other physiological problems — though many go undiagnosed. The Centers for Disease Control and Prevention reports that 37 percent of us get less than seven hours a night, generally considered the tipping point for health problems. Nearly 20 percent of us work shifts with schedules that throw sleep cycles off kilter.
“We’ve become a 24/7 culture,” says retired Cornell psychologist James B. Maas, who helped found the field of sleep education back when TV stations signed off at midnight. “We have to learn to value sleep.”
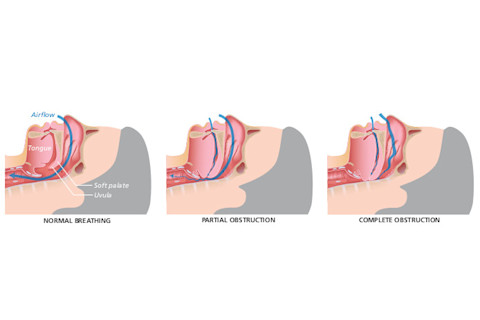
Uninterrupted breathing is crucial for restorative sleep, but the airflow in individuals with obstructive sleep apnea can be completely cut off by soft tissue in the mouth and throat. Harder to diagnose but often as debilitating, upper-airway resistance syndrome is a partial obstruction of the airway. Alila Medical Media/Shutterstock
The struggle to understand sleep apnea and related conditions, known collectively as sleep-disordered breathing, is a major battlefront in the current sleep-science revolution. A seminal moment came in 1998, when pediatric pulmonologist and sleep specialist David Gozal published a study showing that children with OSA were at greater risk of having trouble learning.
Gozal, then director of sleep medicine at Tulane University, took 297 New Orleans first-graders who were performing poorly at school and screened them for apnea. Eighteen percent tested positive — about six times the normal rate. The tonsils and adenoids of 24 of those students were removed, the standard treatment for sleep apnea in children. The parents of the other 30 declined the surgery. Among the treated students, average grades rose significantly the following year, while the untreated kids, along with a control group without OSA, showed no academic improvement.
“I have 24 nice letters from parents thanking me,” says Gozal, who’s now at the University of Chicago Medical Center.
OSA was already thought to be associated with high blood pressure in adults, though the reasons were unclear. Gozal wondered if the same mechanisms might also be driving the correlation between OSA and learning difficulties. As a first step toward finding out, he subjected sleeping rats to bouts of hypoxia, or partial oxygen deprivation, that mimicked apnea episodes. EEG readings showed patterns of sleep disruption similar to those of human OSA sufferers. Afterward, the animals had trouble navigating a water maze. Tissue analysis showed they’d lost neurons in brain regions associated with learning and memory.
In the early 2000s, researchers led by UCLA neurobiologist Ronald M. Harper detected brain-cell death and white matter injury in adult humans with OSA, in areas controlling not only cognitive functions but also mood, breathing, blood pressure and the nervous system’s ability to coordinate sensory information and movement. Meanwhile, Gozal’s team discovered that rats with simulated OSA, and children with the actual disorder, had elevated levels of inflammation markers that can presage cardiovascular problems. In a landmark 2007 study, they performed tonsillectomies on 26 kids with OSA who showed signs of vascular dysfunction; after the operations cured their sleep apnea, arterial tissue returned to normal in 20 of the patients.
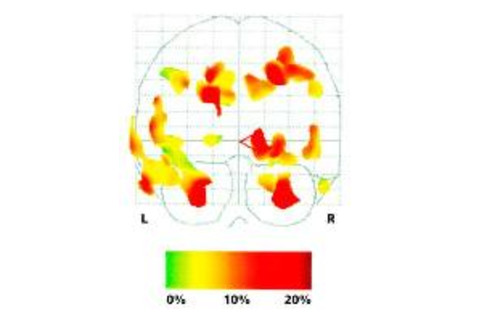
Compared with the brains of normal sleepers, participants with obstructive sleep apnea had reductions in gray matter of up to 18 percent in several regions, according to a 2002 study. Reprinted with permission of the American Thoracic Society. Copyright ©2015. Paul M. Macey, Luke A. Henderson, Katherine E. Macey, Jeffry R. Alger, Robert C. Frysinger, Mary A. Woo, Rebecca K. Harper, Frisca L. Yan-Go, and Ronald M. Harper/2002/Brain Morphology Associated With Obstructive Sleep Apnea/American Journal of Respiratory and Critical Care Medicine/Vol. 166, No. 10/pp. 1382-1387. Official journal of the American Thoracic Society
Gozal’s team eventually found that children with OSA who also had specific gene variants were at particularly high risk for cognitive, cardiovascular or metabolic side effects. And in 2012, they uncovered the first evidence that sleep apnea influences epigenetics, altering gene expression without changing an individual’s DNA. In one kind of epigenetic change, known as DNA methylation, a methyl group (a carbon atom plus three hydrogen atoms) is added to a portion of DNA; it essentially flips a gene’s switch to the “off” position, shutting down the often-crucial function it performs. In children with OSA and elevated inflammation levels, at least one immune-system gene tends to be highly methylated. Hypermethylation can promote tumor growth; that may explain why, in a separate study, Spanish researchers in 2012 found higher rates of cancer among adult sleep apnea patients.
Although the damage caused by OSA comes partly from sharp fluctuations in oxygen levels as the patient fights for breath, much of the disorder’s devastation appears to result from its disruption of sleep. “We’ve separated those elements,” says Gozal. “Fragmented sleep alone is associated with inflammatory processes, oxidative stress and a variety of downstream consequences.”
Dealing With Deficit
Not all sleep deprivation, of course, is caused by disorders such as apnea. Many of us simply go to bed too late or have trouble falling asleep once we get there — a pattern we may repeat night after night. In 1999, University of Chicago endocrinologist Eve Van Cauter published the first study of the metabolic effects of that kind of chronic sleep deficit. At her lab, she restricted 11 healthy young men to four hours of sleep for six nights. For days afterward, the subjects metabolized glucose as poorly as pre-diabetics. Their blood cortisol, a hormone that rises with both stress and aging, reached levels common in much older men.
In later studies, Van Cauter and her colleagues found that men with a sleep debt developed higher levels of the hormone ghrelin, which stimulates the appetite, and lower levels of leptin, which suppresses it. Testosterone levels dropped as well. Such endocrine changes may help explain why epidemiologists have found elevated rates of obesity and diabetes among habitual short sleepers. “An animal will only deprive itself of sleep if it needs more time to forage,” Van Cauter observes. “So the body interprets sleep deprivation as a need to find more food.” In response, our hormones spur us to seek out edibles and store energy as fat.
Eve Van Cauter, director of the Sleep, Metabolism and Health Center in the Department of Medicine at the University of Chicago, leaves a sleep study lab after meeting with a participant. Brett Roseman
As it sends the nervous system into emergency mode, sleep deprivation does other kinds of damage. It can trigger widespread inflammation, which is the immune system’s response to a generalized threat, even as it decreases that same immune system’s ability to target specific viruses. As a result, sleep-deprived people have been shown to respond less robustly to vaccinations and to catch more colds. Inflammation also erodes telomeres, the “caps” at the ends of chromosomes that protect genes from degradation, which can lead to early cell death, premature aging and even cancer. Several recent studies report that telomeres are shorter among undersleepers. The risk of depression — another disorder associated with inflammation — is 16 times greater after a year of insufficient sleep, according to a 2013 study by UCLA psychoimmunologist Michael Irwin.
Sleep doesn’t just allow the body to focus on rebalancing hormone levels and hunting down pathogens. It also enables the brain to do some crucial housecleaning — cognitive and otherwise. Many experiments have shown that when people or animals learn a skill, they perform it better after a good sleep. Some of this memory consolidation may occur through dreaming. For example, EEGs indicate that sleeping rats replay the running of a maze in a brain region devoted to spatial learning. But the brain during sleep also appears to erase some memories to preserve others. How this might work was first sketched out in 2003 by University of Wisconsin psychiatrist and neurobiologist Giulio Tononi. He theorized that the brain becomes overloaded with new neuronal connections — or synapses — during waking hours, as an animal absorbs information. To prune excess connections, the sleeping brain weakens each synapse by a proportional amount so that only the strongest survive, Tononi suggested.
His hypothesis was confirmed in an experiment conducted by Paul Shaw, a neurobiologist at Washington University in St. Louis. Shaw exposed fruit flies to an environment rich in social interaction and counted their synapses before and after; as expected, the flies grew lots of new connections. Then he let them sleep for as long as they wanted, which proved to be longer than usual, suggesting that they needed time to consolidate what they’d learned. When the flies awoke, Shaw found, the number of synapses was greatly reduced, just as Tononi would have predicted.
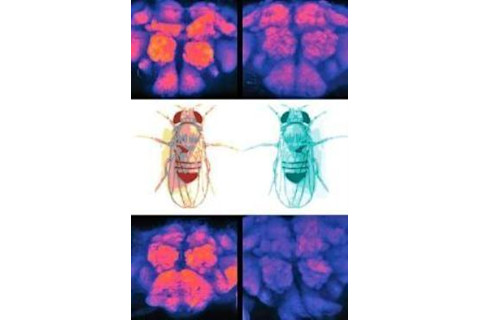
Synaptic connections (shown from different angles, top and bottom) developed during a fruit fly’s waking hours (left) were pared down after sleep (right), confirming that the brain does some housecleaning during slumber to keep only the most useful connections. Chiara Cirelli
University of Rochester neuroscientist Maiken Nedergaard recently revealed another way the brain tidies up during sleep. In a 2012 paper, Nedergaard and her colleagues announced the discovery of a waste-disposal system in the brain, in which toxic metabolites such as beta amyloid — associated with Alzheimer’s and other neurodegenerative diseases — are flushed out by cerebrospinal fluid with the help of support cells called glia. In 2013, the team released a mouse study showing that this system turns on during sleep.
“It’s been known for years that diseases like Alzheimer’s are associated with sleep disturbances,” Nedergaard says. “But maybe physicians should be treating sleep to slow the progression of the disease.” Indeed, she notes, a 2009 study at Washington University found that sleep-deprived mice developed Alzheimer’s-like brain plaques more often than their well-rested cousins. “Because it fits, right? If you don’t sleep, you don’t clean your brain.”
Joe Borelli is evidence of that assertion.
Within months of beginning his second round of CPAP treatment in 2009, Borelli was feeling more rested than he had in ages. The symptoms that dogged him for five years — the memory lapses, anxiety, clumsiness, heart palpitations and all the rest — began to vanish. So did his high blood pressure.

Before diagnosis and treatment, Borelli was forced to give up many of his professional and personal interests because of the health problems caused by upper-airway resistance syndrome. But now he’s back in the game, shown here during practice at a South Carolina tennis club. Sean Rayford
Borelli, 53, went on to create an app, known as SleepMapper, to help other CPAP users optimize their therapy. And although his mental acuity isn’t quite what it was before years of cumulative damage from his sleep disorder, he’s not complaining. “I lost 50 percent of my brain to this disease,” he says, “but I got 90 percent back. I’m a happy, happy camper.”
[This article originally appeared in print as "Wake-Up Call."]














